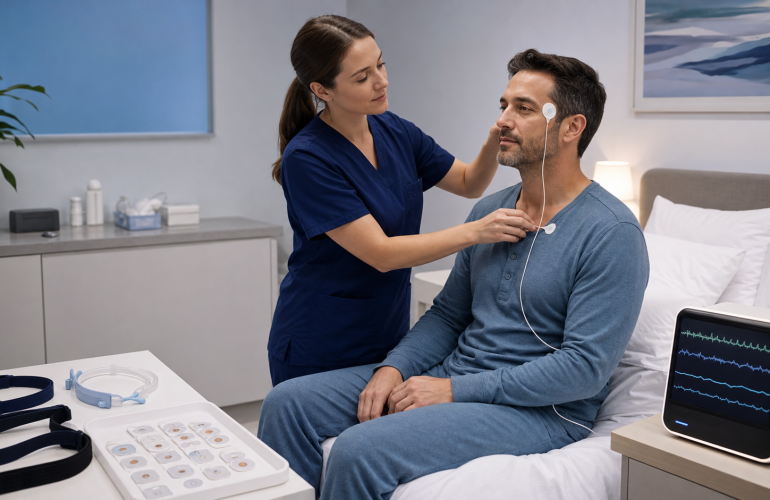
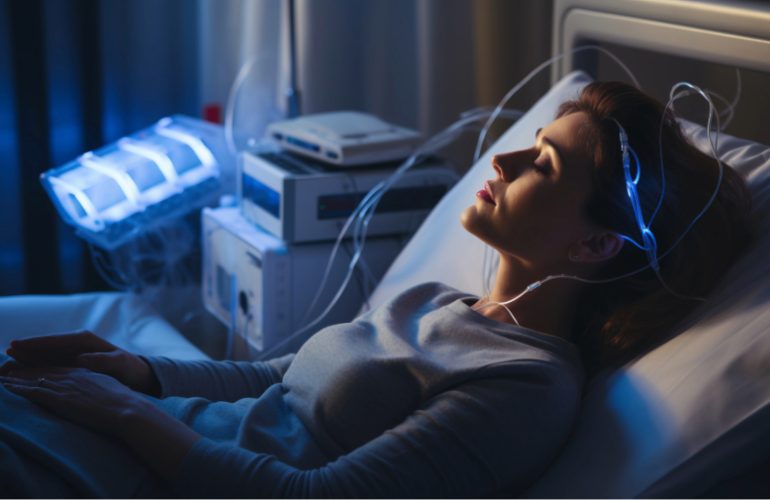
Sleep disorders are common and not only do they disrupt your sleep, they can truly impact your quality of life. They can also affect your partner’s sleep as well. To receive an official sleep disorder diagnosis, your primary care physician will likely refer you to a sleep professional for an in-laboratory sleep study test known as polysomnography.
What is a Sleep Study (Polysomnography)?
A polysomnography (PSG) is a type of sleep study. The true polysomnography definition is it’s a multi-parametric test sleep professionals use as a diagnostic tool to study sleep in sleep medicine.
A polysomnography is used for diagnosing various sleep disorders typically in settings such as a:
- Sleep center
- Free-standing facility
- Hospital
- Dedicated sleep clinic
Types of Sleep Studies
There are four main types of sleep study tests, as overviewed below. This article describes the diagnostic overnight Polysomnography (PSG) in depth, while we will go over the other types of sleep studes in future articles.
1. Diagnostic Overnight Polysomnography (PSG)
A test used to monitor sleep and certain functions of the body during sleep such as:
- Blood oxygen levels
- Limb movements
- Breathing patterns
- Heart rhythms
2. Diagnostic Daytime Multiple Sleep Latency Test (MSLT)
A test sleep professionals use for diagnosing narcolepsy. They also use it to measure your degree of sleepiness during the day. It measures how fast you fall asleep during the day in quiet situations as well as monitors how fast you enter REM sleep and how often. A sleep technologist will perform this test on the morning after you’ve received a diagnostic overnight PSG.
3. Two-night Evaluation PSG and CPAP Titration
You’ll receive diagnostic evaluation and general monitoring your first night. If it’s discovered you have sleep apnea, the sleep physician will ask you to come back a second night to figure out what air pressure is adequate for your continuous positive airway pressure (CPAP) treatment. This is a device that delivers air through a special nasal mask into your airways.
4. Split-night PSG with CPAP Titration
A test conducted when you have or it’s highly suspected you have moderate to severe sleep apnea. The sleep professional uses the second half of the night to figure out the required CPAP pressure to offset your apnea.
5. Home Sleep Apnea Test (HSAT)
Your doctor may allow you to use an at-home sleep study test to diagnose obstructive sleep apnea (OSA) rather than you going to the sleep center. Either a technologist will come to your house to set the device up for you or you can pick it up at the sleep center. You may use at-home sleep study testing when:
- You’re under a sleep specialist’s care
- You don’t have other sleep disorders
- Your doctor believes you have high probability of having OSA
- You don’t have lung disease, heart disease or any other serious health problem
Reasons for Polysomnography (Sleep Study)
According to the AAST, the reasons for getting a sleep study or polysomnography include having:
- Periodic limb movement disorder
- Sleep apnea
- REM sleep behavior disorder
- Narcolepsy
- Unexplained chronic insomnia
- Unusual behaviors during sleep
- Circadian rhythm sleep-wake disorders
- Obstructive sleep apnea
- Idiopathic hypersomnia
- Parasomnias
- Mixed or complex sleep apnea
- Central Sleep Apnea
Although this isn’t an exhaustive list, it does represent more than a handful of the most common sleep disorders doctors need to rule out.
Sleep professionals use polysomnography not only to help them diagnose numerous sleep disorders, but also to help them learn if they need to adjust treatment plans or if the treatment plan being used is already effective.
The polysomnography provides sleep technologists with specific information through observation and equipment that includes:
- Brain waves (EEG)
- Blood oxygen levels
- Leg movements
- Breathing patterns and rates
- Eye movements
- Body positioning
- Sleep stages
- Heart rhythms and rates
- Unusual behaviors or movements
- Noises and snoring made while sleeping
This is all done while you’re sleeping. Once the technologist collects the information, they’ll evaluate and chart this information.
Indications for a Sleep Study
The PSG often evaluates for sleep apnea symptoms such as:
- Loud and ongoing snoring
- Daytime sleepiness despite being rested
- Frequent nighttime wake up episodes
- Holding your breath for periods of time while you sleep that follows with gasps of air
- Restless sleep
The National Heart, Lung, and Blood Institute (NHLBI) warns that leaving sleep disorders untreated could increase your risk of high blood pressure, heart disease and stroke. There’s also an association between sleep disorders and a higher risk of car accident-related or fall-related accidents.

Preparing For and During Your Sleep Study
Your doctor will likely ask you to refrain from drinking alcohol, eating or drinking anything that contains caffeine the day before your sleep study. Caffeine and alcohol could change your patterns of sleep and could also worsen your sleep disorder symptoms.
You’ll arrive in the evening at the sleep laboratory for your sleep study test and stay overnight. You’re encouraged to bring regular bedtime routine items like your nightclothes. The polysomnography room is kind of like a hotel room and is quiet and dark during your test. It has its own bathroom and you don’t share your room with anybody.
You’ll have a video camera in your room so the sleep technologists can monitor you and see everything that’s going on in your room once the lights are out. You’ll also have an audio system in your room as well so they can hear and talk with you from their monitoring station outside your room.
Once you’re ready for bed, a technologist will use a mild adhesive to attach sensors to different areas of your body such as your:
- Chest
- Scalp
- Legs
- Temples
They connect the sensors to a computer by wires, but you can still move around in bed since the wires are long enough. They’ll also place a small clip on your ear or finger to monitor your blood oxygen level.
What Happens During an Overnight Polysomnogram Sleep Study?
Polysomnography is a painless, noninvasive test. It’s rare to have complications. You may experience minor skin irritation due to the adhesive used for attaching the testing sensors to your skin. It’s discouraged to take a nap the afternoon before you have the sleep study.
The sleep technologist will evaluate the information gathered first and use the data to chart your sleep cycles and stages. Then a sleep center doctor will review the information.
It could take a couple weeks before you receive your polysomnography results. You’ll need a follow-up appointment so your doctor can go over your results with you. They’ll then go over your treatment plan or further evaluate you, depending on the data gathered.
If your doctor gives you a sleep apnea diagnosis, they’ll likely prescribe you a CPAP machine where you’ll receive a constant delivery of air to your mouth and nose while you’re sleeping. You may require a follow-up polysomnography to determine which setting on your CPAP machine is right for you. If you receive another sleep disorder diagnosis, your doctor will provide you details on the right treatment options.
If other types of sleep disorders are diagnosed, you may receive a combination of western medicine and holistic methods to improve your sleep quality.
As newer technologies evolve, the sleep industry will likely evolve too. Improved methods to measure and quantify sleep can help with better sleep disruption assessment, leading to better recognition of new types of disorders and better outcome predictions.
Ready to End your Sleep Disorder Problems?
To find out if using Western medicine and/or holistic measures are the answer to your sleep struggles, contact us here at Sweet Sleep Studio LLC today for a consultation. Dr. Abid Bhat, MD MBA, Sleep Medicine Specialist, and his team are standing by to help you with your sleep disorder-related questions and concerns. We’re committed to your improved sleep and health. Our mission is to help people sleep better and maintain a positive state of mind and body so they can enjoy life more.